INESS has released a new publication entitled Missing Health Professionals: 21 Improvements.
DOWNLOAD THE PUBLICATION IN SLOVAK [PDF]
The number of health professionals is a globally discussed issue. The WHO expects 18 million missing health professionals by 2030, mainly in lower- and middle-income countries. Two out of five active doctors in the United States will be 65 years of age or older in the next decade.
In Germany, 14,000 nursing positions in hospitals and another 8,000 in intensive care units were unfilled in 2021, when it comes to doctors, it was 5,000 positions. Almost half of general practitioners in France reported in 2019 that they were no longer accepting new patients.
While the number of doctors in Slovakia has increased by approximately 13% in the last 12 years, the number of nurses has decreased by approximately 3%. The proportion of doctors aged 65+ has increased from less than 7% in 2009 to more than 16% in 2020. The proportion of younger doctors is at least being maintained or slightly increased.
However, in contrast to doctors, the proportion of younger nurses is significantly declining. The under 40 years of age category accounted for almost 44% of nurses in 2009, but only 22% in 2020. There is larger number of doctors in the Bratislava region (more than 6 doctors per 1,000 inhabitants) compared to other regions (2.5 – 4 doctors per 1 000 inhabitants). While in 2009 there were 27 doctors and 49 nurses per 1 000 people aged 65+, in 2020 there were only 22 doctors and 34 nurses.
Simple Solutions Do Not Exist
Universities, higher wages, or technologies are often discussed as the solutions to this problem. Health sciences graduates accounted for 4% of graduates in Slovakia 10 years ago, and today, they account for up to 8% of all graduates (after deducting foreigners). If we look at medical sciences alone, the share of 1.5% in 2010 has risen up to 2.7% in 2020.
Thus, increasing vacancies for students in medical faculties alone will only have a limited effect. The proportion of secondary school students who want to pursue a career in health care, especially medicine, cannot grow indefinitely.
We have divided the steps to improve this into two subgroups. One is extensive, dealing with quantity, i.e. how to increase the absolute number of health professionals, or at least maintain or slow their decline. The other deals with intensive changes, i.e. how to produce more services without the need to supply more workers of today’s typical medical qualifications.
Two facts appeared on the issue of wages of health professionals in Slovakia. Firstly, the average wages of health professionals have grown at above average over the last 15 years. Secondly, wage growth will have to continue despite the global competition and the fact that these wages will drain an increasing proportion of healthcare finances.
Average wages of doctors are roughly three times the average wage in the economic sector. Wage growth for nurses has been significantly slower, but still above the labor market average. Wages of health professionals will continue to rise, but the economic scope for further acceleration of this growth is already limited.
Artificial intelligence, big data, e-health, wearables, robotics, and other innovations have the potential to improve workforce utilization. But looking at recent history, we must conclude that we should expect evolution rather than revolution. The real challenge often lies not in discovering but in bringing a new concept to life.
There are no easy solutions to the shortage of health professionals. But there are improvements.
21 Improvements for Better Access to Health Services
A new INESS publication entitled Missing Health Professionals: 21 Improvements provides a summary of the current situation as well as a reflection on the content of the term “shortage”. The main part of the publication is the 21 concrete suggestions for improvement. They are divided into two groups.
Extensive:
- Reform of medical education and attestation
- Reflecting the Supreme Control Office (NKU) report on residency and setting the final goal
- Explore the possibility of increasing the capacity of secondary medical schools
- Reflect the findings of the Supreme Control Office (NKU) on secondary health education
- Analyze obstacles to further development of part-time health care
- Developing a strategy for the recruitment of Roma health professionals
- Gradual withdrawal from the payroll system
- Improvement of regulatory conditions for the development of health centers and ambulance networks, enabling the emergence of more types of contractual networks
- A program for the smooth entry of third-country health professionals into Slovakia, especially Ukrainian refugees
Intensive:
- Regular reassessment of the competencies of all people in the sector to increase participation, including education conditions. The involvement of a large network of pharmacies in health care delivery and a reassessment of mandatory education and roles of junior health staff could be a starting point.
- Regular auditing of bureaucratic obligations in the health sector and their elimination
- Introduction of fees at least in the most problematic sectors (ambulance services, etc.)
- An alternative to a fee for the medical referral letter
- Gradual building of claimable waiting periods
- Simplification of administrative access to treatment (prescribing and indication restrictions)
- Mandatory remote interview (phone, application) before a free doctor’s visit
- Developing the possibility of aliquot reimbursement of relevant procedures in Slovakia and abroad
- Significant strengthening of teaching about health and the human body in schools
- Creating the legal and moral space for family members to be involved in healthcare
- Preparing the legislation for more flexible forms of contracts between providers and health professionals
- Technology thrives in a system where innovations are not controlled from above, but is sought after by system participants themselves because it gives them a competitive advantage. The spread of innovations in healthcare therefore needs a less directive and more competitive view of the system.
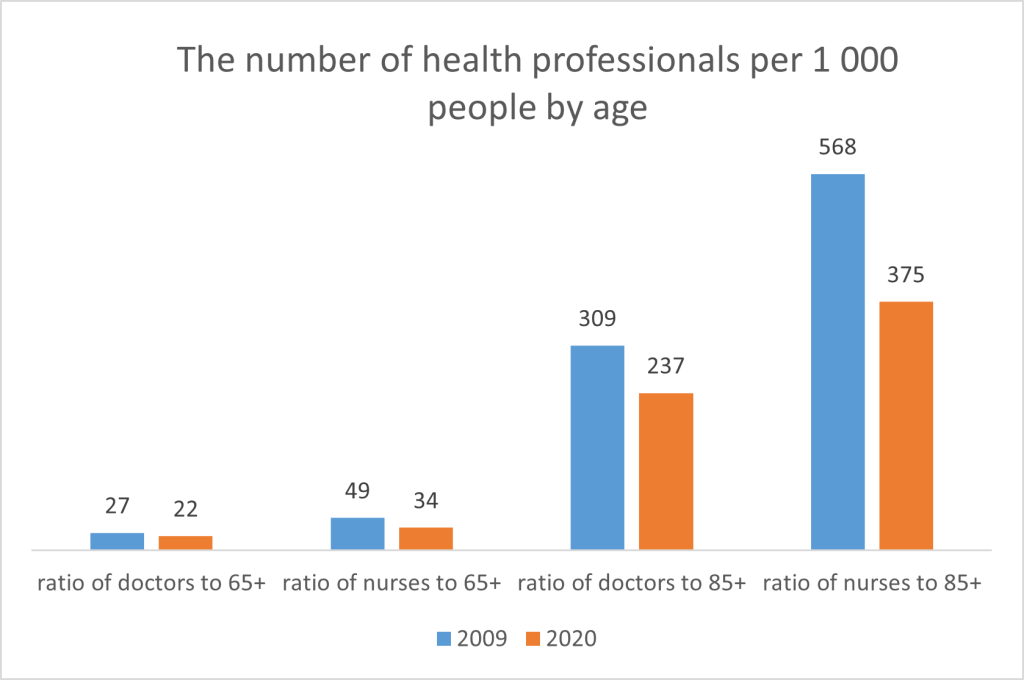
Source: INESS
Continue exploring:
Day of Respect for Taxpayers: We All Are VIP Clients of Public Institutions



